2Ministry of Health, General Directorate of Public Health, National Molecular Microbiology Reference Laboratory, Ankara, Türkiye
3Department of Medical Microbiology, Kayseri City Training and Research Hospital, Kayseri, Türkiye
4Intensive Care Unit, Kayseri City Training and Research Hospital, Kayseri, Türkiye
5Department of Anesthesia and Resuscitation, Kayseri City Training and Research Hospital, Kayseri, Türkiye
Abstract
Objective: Carbapenem-resistant Klebsiella pneumoniae (CRKp) is associated with high mortality rates due to carbapenemase production. Türkiye is endemic for oxacillinase-48–producing carbapenemase (OXA-48), and New Delhi metallo-β-lactamase-1 (NDM-1) has also recently emerged. This study aimed to investigate mortality risk factors and carbapenemase types in patients with CRKp bacteremia.
Materials and Methods: This prospective study included 83 adult patients with CRKp bacteremia at Kayseri City Training and Research Hospital between September 2023 and March 2024. The control group consisted of patients without infection from the same hospital units. Pathogens were identified using the Vitek 2 system. Susceptibility to ceftazidime-avibactam and colistin was determined using disk methods. Carbapenemase genes were detected by polymerase chain reaction (PCR).
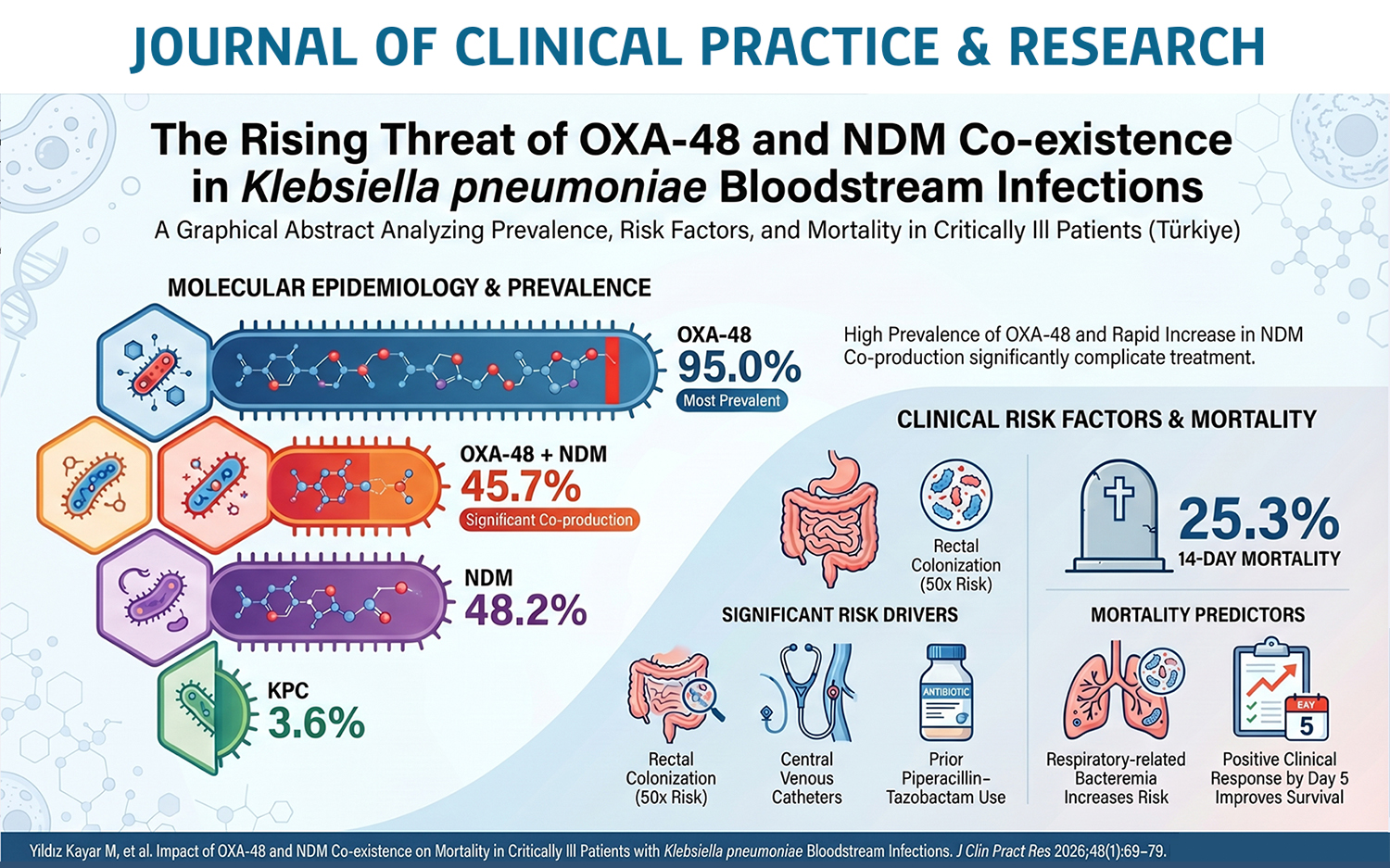
Results: In the multivariable logistic regression analysis, central venous catheter use, rectal colonization, and prior piperacillin–tazobactam use were identified as significant risk factors for CRKp bacteremia. Among the isolates, 95% carried OXA-48, 48.2% carried NDM, and 3.6% carried Klebsiella pneumoniae carbapenemase (KPC); OXA-48 and NDM co-production was detected in 45.7% of isolates. Verona integron-encoded metallo-β-lactamase (VIM) and Imipenemase metallo-β-lactamase (IMP) were not detected. Fourteen-day mortality was 25.3%. Respiratory system-related bacteremia was identified as an independent predictor of mortality, whereas clinical response on day 5 was independently associated with lower mortality. No difference was observed between monotherapy and combination therapy.
Conclusion: This study demonstrates that OXA-48 remains the most prevalent carbapenemase type in CRKp bloodstream infections in Türkiye, while NDM is increasing rapidly and frequently co-occurs with OXA-48, worsening clinical outcomes. Strengthening infection control measures, promoting the prudent use of antibiotics, and ensuring access to new treatment agents are crucial for reducing the spread and impact of CRKp infections.
Graphical Abstract